by Dr. Heath McKinley
Share
by Dr. Heath McKinley
Share
Why Your Neck Pain Keeps Coming Back
I’ve been doing this for 25 years in North Center. When someone walks into my office with neck pain that keeps returning, they’re usually frustrated. Not just because of the pain itself, but because of what it’s preventing them from doing: playing with their kids without wincing, getting through a workday without constantly adjusting their position, sleeping through the night, or running and golfing like they used to.
And I already know what the conversation’s going to sound like.
They tried rehabilitation. It helped for two weeks.
They got a massage. Felt great that afternoon, stiff again by morning.
They took muscle relaxers. The pain went away. Then it came back.
The pattern is always the same. Temporary relief followed by recurrence. And the reason is simple: they treated one layer of the problem while the other layers stayed compromised.
Your neck pain isn’t just about your neck. It’s about what accumulated over years: screen posture, sleep position, old injuries, compensatory movement patterns. All of it creates a cascade effect that single-technique approaches can’t touch.
The Text Neck Epidemic Nobody’s Measuring
When I started practicing in 2002, I’d see degeneration patterns in patients’ late thirties. Disc height loss. Forward head posture. Early arthritis.
Now I’m seeing the same patterns in 18, 19, 20-year-olds.
Normal and common are two different things.
The difference? Smartphones and computers. Research shows that U.S. adults spend an average of 7 hours and 2 minutes on screens daily. College students push that to 8-10 hours per day on smartphones alone.
That’s 40 to 60+ hours a week at computers for work, plus constant phone use, especially at night, right next to the bed. The forward flexion of looking down or texting has become so prevalent that 60.8% of university students now show text neck syndrome.
This is on top of everything that existed before the smartphone era.
Here’s what most practitioners miss: that forward head posture while reading or texting places mechanical demand on neck muscles 3-5 times that of a neutral neck posture. It’s like what a dentist sees when they look at your teeth: things accumulate over time, plaque builds gradually until your body gives you a signal. The same thing happens with tension and degeneration in your neck until the structure can’t hold anymore. That’s what I see on EMG testing: muscle tension 40 times above normal.
The body’s ability to handle any new stress becomes almost zero.
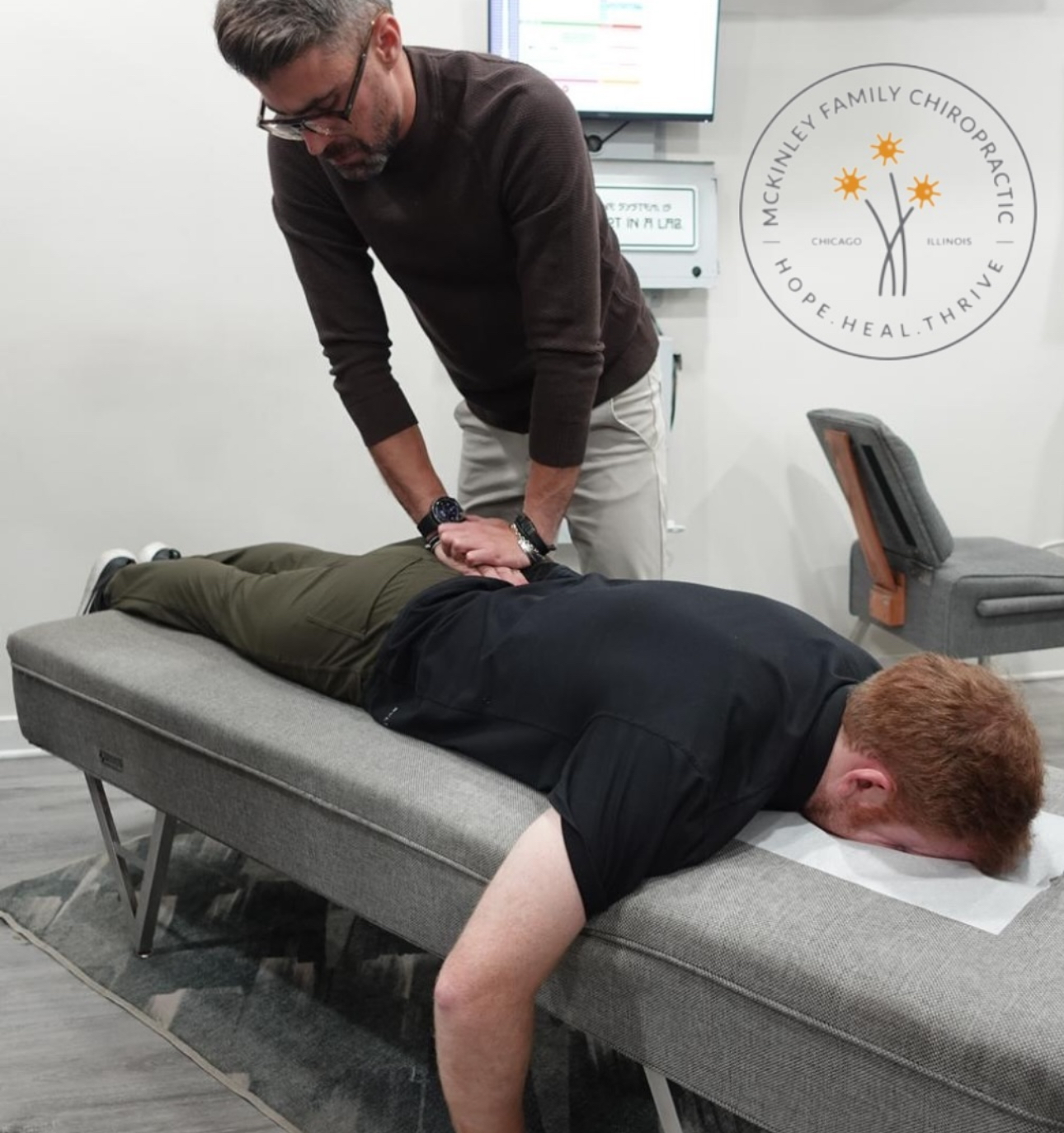
Why Single Adjustments Fail
When you come in with neck pain, most practitioners will adjust your neck. Maybe they’ll work on your upper back. You’ll feel better for a few days, maybe a week.
Then it comes back.
The reason? They addressed one compromised layer. The structural misalignment got corrected temporarily. But the neuromuscular tension stayed elevated. The movement patterns that created the problem in the first place never changed. Your sleep position kept reinforcing the forward head posture.
You can’t fix a multi-system problem with a single-system solution.
In our office, before we do anything, we run a comprehensive assessment. Not just range of motion (though we do that across your entire spine, hips, and knees, because they’re all connected). We take X-rays to see structural alignment, disc height, loss of cervical curve. We use EMG testing to measure neuromuscular tone across your entire spine, not just where it hurts.
We also measure muscle symmetry with InBody scanning. If one arm is losing muscle mass, or if your body composition is shifting in ways that signal dysfunction, we need to know that before treatment starts.
This gives us objective baselines. We’re not guessing whether treatment is working. We’re measuring it every 30 days.
And here’s what I find in almost every case: the problem isn’t isolated to the neck. The tension patterns run through the upper cervical and lower back. The curve is flattened. The disc space is narrowing. And the muscle tone is so elevated that the body has almost no capacity left to adapt.
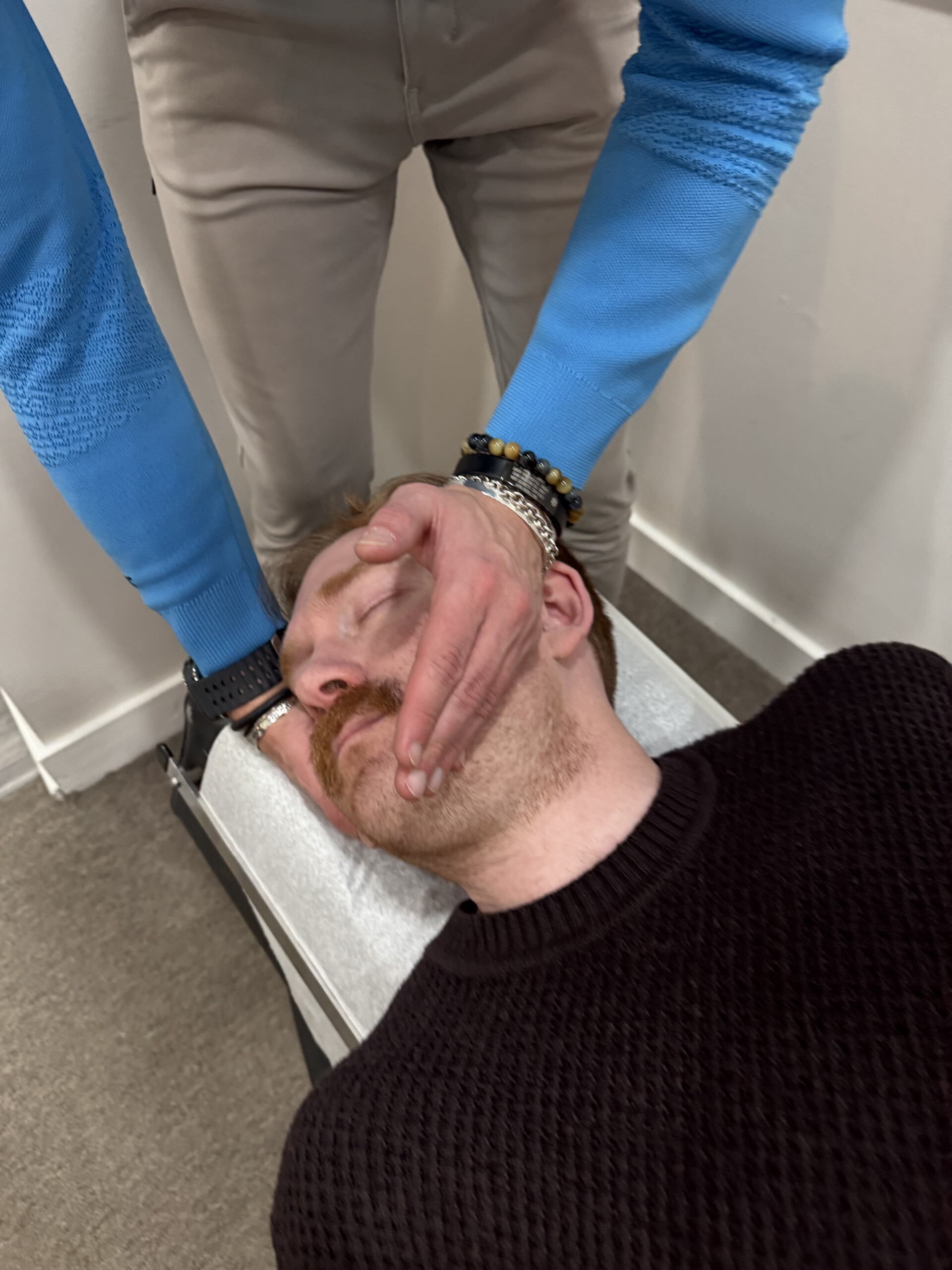
The Carpal Tunnel Misdiagnosis
One of the most common patterns I see: someone comes in for neck pain. During the assessment, I ask about numbness or tingling in their hands.
“Oh yeah, I get that at night. My doctor said it’s carpal tunnel. I’m wearing wrist guards.”
Carpal tunnel syndrome is probably the most misdiagnosed orthopedic condition in the world. And it frustrates me every time I see it. That’s why so many people are walking around in those black wrist guards that don’t help.
Most of the time, the numbness into the hands isn’t coming from the wrist. It’s coming from cervical compression in the neck. The same nerves that are causing your neck pain are also being pinched higher up in the spine, and you’re feeling it in your hands.
This is classic text neck.
When we correct the neck dysfunction (realign the cervical spine, reduce the neuromuscular tension, restore proper movement patterns), the hand numbness resolves. Not because we treated the wrist. Because we addressed the actual source.
I tell patients this in advance. Before we start treatment, I predict what’s going to improve beyond the neck pain. Sleep quality. Hand numbness. Shoulder tension. Sometimes even sinus drainage, because when we reduce the muscle restriction in the upper cervical region, it improves lymphatic flow and drainage patterns.
When those secondary improvements happen exactly as I said they would, patients understand this isn’t coincidence. It’s cause and effect.
What Comprehensive Assessment Actually Reveals
Here’s my favorite analogy for how the body works: the fuse box.
After a storm, you might overload a circuit in your house. You go down to the basement, flip the breaker, and the kitchen works again. The electrical current recalibrates.
Your body operates the same way. The brain sends messages down the spinal cord and out through 31 different nerve roots. If there’s irritation or compression creating neck pain, those same nerves are also being compressed. And wherever those nerves go, you’ll feel an effect.
Not all of those effects show up as symptoms people would connect to their neck. That’s why someone comes in for neck pain and I’m asking about their sleep, their digestion, whether they wake up stiff, whether they’re tossing and turning at night.
When I explain this during the initial consultation, most people aren’t skeptical. We do a good job of explaining it. But you will find the occasional skeptic, and those patients usually become the best referral sources. Because when you surprise a skeptic, they tell everyone.
The data backs this up. Research shows that 30% of patients with neck pain will develop chronic symptoms, and nearly 50% will continue to experience some degree of pain or frequent occurrences. That’s because single-technique approaches almost always lead to recurrence.
The best outcomes come from combining multiple therapeutic techniques. That means correcting your posture while also stabilizing the shoulder blade. Manual adjustments combined with exercises that retrain how your body moves. Not one thing. Multiple things working together.
That’s exactly what we do. The combination of techniques we use depends on your age, your history, how much degeneration you have, and how your body responds.
The Recalibration Process
When we start treatment, I tell patients upfront: your body may adapt similar to a new exercise program. You might feel a little sore in the first 24 hours. But it’s going to feel more like exercise soreness than pain.
As you improve, you’re probably going to sleep better. You might notice the hand tingling stops. Your shoulder tension eases. Maybe your sinuses drain better.
And here’s the part most practitioners don’t explain: as your nervous system recalibrates, you might have temporary flare-ups. That doesn’t mean treatment isn’t working. It means your body is resetting itself.
We’re not masking symptoms. We’re retraining your nervous system to function properly again.
Most people see measurable improvement within the first week or three adjustments. Real chronic cases might take two weeks or six visits to start noticing the difference. By 30 days, we have objective data showing improvement on EMG tests and other assessments.
Once you’re out of the acute phase (pain’s gone, sleep is better, secondary symptoms have resolved), we transition to wellness care. How often depends on how your scores look. If your EMG was 40 times above normal and we’ve gotten you down to 4 times above normal, you might still need to come in once a week for a month or two to get you as close to normal as possible.
Then we move into maintenance. For most people, that’s once a week to twice a month. People who are more active, or who have underlying conditions that make it hard to get to 100%, might need more frequent visits.
Now, not everyone continues with maintenance. Some people feel better and stop coming. That’s their choice. And when they come back six months or a year later because something flared up again, I never say “I told you so.” I just help them get better again. But what they usually notice is how quickly their body recovers this time, because we’ve already trained it once.
The goal is prevention. Not managing flare-ups.
Prevention: What You Can Do at Home
Once we’ve gotten you out of that acute phase and your nervous system is recalibrated, prevention becomes the focus. And there are practical things you can do at home to support that.
I’m 51. I work out every day. Golf, basketball, weights. I’ve raised three kids without medication. I know what I’m asking you to do because I do it myself.
Most of our patients do inversions at home. Not an inversion table, just simple hanging exercises. You can arch in a doorway or hang off the edge of your bed with the edge near your shoulders. Twice a day for about 60 seconds, usually morning and evening. These exercises create gentle extension and traction, countering the constant forward flexion from screens.
Think of it like brushing your teeth. You’re not brushing because you have a cavity. You’re brushing to prevent one from developing. The inversions work the same way: they maintain the structural corrections we’ve made in the office.
These five-minute exercises help offset that forward head posture from computer and tech use. Once we’ve measured your progress and confirmed you’re balanced, these become part of your daily routine.
The other big one: stop charging your phone next to your bed.
Put it in the kitchen. Make yourself get out of bed to check it.
We find that people who do this improve their sleep quality significantly. That’s critical for healing. But it’s also that many fewer hours looking down at a screen, reinforcing text neck right before sleep and in the middle of the night.
Movement is life. If you’re not moving, things break down faster. But more importantly for neck pain, regular movement reinforces the proper patterns we’re retraining in the office. It prevents your body from defaulting back to the compensatory movements that created the problem in the first place.
Stay active: 20 to 30 minutes minimum, five to six days a week. Drink enough water so you don’t get dehydrated, which increases cramping and muscle contracture.
And get out into nature. We practice in a city environment. Being outside reduces stress, which directly lowers muscle tension, and it usually means less screen time, both of which support long-term neck health.
Why It Keeps Coming Back (And How to Stop the Cycle)
Your neck pain keeps coming back for the same reason most chronic problems persist: you’re treating one layer of a multi-layer problem.
The massage relaxed the muscles but didn’t address the structural misalignment. The adjustment corrected the spine temporarily but didn’t retrain the movement patterns that pulled it back out of place. The muscle relaxers masked the symptom while the nerve compression continued.
And nobody measured what was actually happening underneath.
Text neck from 40-60 hours of screen time per week doesn’t resolve with a single technique. Forward head posture that’s been building for years doesn’t correct itself after one visit. Neuromuscular tension at 40 times normal capacity doesn’t release because you stretched for five minutes.
The solution isn’t doing more of what already failed. It’s comprehensive assessment followed by multi-system treatment.
Most people start feeling better within the first week. By 30 days, we have data showing what changed. And the only thing you’re going to be mad about is that you didn’t know me sooner.
Your body already knows how to heal itself. It’s been trying to heal for years. Our job is to remove the interference so it finally can.
Why Most Sciatica Patients Are Told to Wait When Diagnosis Should Come First Most sciatica patients are told to wait, take anti-inflammatories, and hope it gets better. If it doesn’t, they get sent to physical therapy. Then imaging. Then maybe a specialist who mentions cortisone or surgery. Here’s what almost never happens: someone asks why […]
Chiropractic Care and Quality of Life Among Office Workers With Nonspecific Pain Office workers commonly experience neck pain, back discomfort, headaches, and muscle tension as a result of prolonged sitting, poor posture, repetitive movements, and daily stress. These symptoms are often classified as nonspecific musculoskeletal pain, meaning pain that is not linked to a specific injury […]